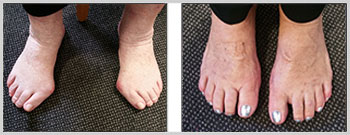
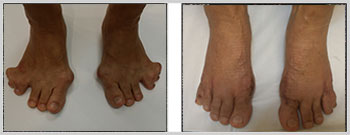
Bunion
Bunion (Hallux Abducto Valgus) Surgery
The amount of information available regarding bunion surgery is exhaustive, and can be confusing. This section has been designed to cut through the clutter and false information.
Most people that are referred to CPSM by their podiatrist have exhausted conservative options, and are recommended surgery to prevent further joint deformity and joint destruction. If you have tried conservative care, and the bunion is causing pain or limiting your activity, surgery can be a very effective option.
What is a bunion?
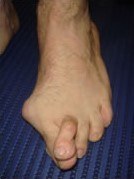
The medical Latin term for a bunion is Hallux (big toe) Abducto (big toe moving towards the 2nd toe) valgus (big toe rotates inward). It is characterised by a deformity of the first metatarsophalangeal (MTP) joint with lateral deviation of the big toe and a large medial prominence (bump) at the first metatarsal head which eventually leads to joint degeneration and cartilage wear (arthritis). Bunions are almost always hereditary and can be worsened by contemporary shoes and abnormal mechanics of feet. A bunion is not an abnormal growth on the side of your foot, but a mal-alignment of your big toe joint. The bones that make up your big toe joint, are no longer aligned straight, but are moving in opposite directions, causing the prominence that you see.
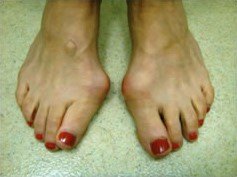
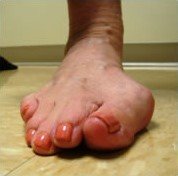
When should you have bunion surgery?
At the Centre for Podiatric Surgery & Medicine (CPSM), we use the following criteria as a guideline when determining if surgery is indicated:
- You have a bunion - with progressive arthritis confirmed by clinical exam and x-rays
- You feel you have exhausted all conservative care. Conservative therapy may include the following and can be provided by your podiatrist
- Functional orthotics prescribed and cast by your podiatrist and designed to relieve pressure within the big toe joint
- Shoe Therapy, including proper shoes for your foot type and activities and possible modifications to your shoes
- Accommodative padding
- Activity modifications
- Medications - short term therapy may help to reduce inflammation
- Injection therapy - rarely used but may help in treating an inflamed bursa
- Bunion interferes with daily activities
- Pain inside the joint
- You would like surgery sooner than later
The surgical procedure
There are more than 100 different ways to perform bunion surgery. The best procedure for one person is not necessarily the best for another. Some procedures allow you to walk much sooner meaning you may not have to use crutches. Depending on your foot type the procedure can have a greater risk for return of the bunion deformity. Other procedures may require you to be on crutches for few weeks - but may offer a better long-term result.
Types of bunion surgery:
Generally, bunion surgery can be classified into two major categories:
- Head procedures (around the great toe joint)
- Base procedures (near or at the joint behind the great toe joint)
For a Head procedure, the bone is cut and the head of the metatarsal moved over to correct the bunion. Various types of bone cuts can be performed depending on the necessary correction. Head procedures are usually indicated for a mild to moderate bunion, or for patients who do not feel they can be non-weight bearing for any length of time.
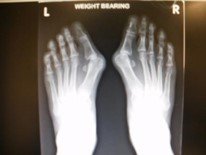
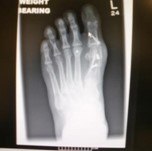
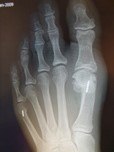
Pre-operative x-rays show a very mal-aligned big toe joint. The same patient underwent a head procedure, a scarf /Akin osteotomy. Far right is an Austin style bunionectomy.
Base procedures are performed around the base of the 1st metatarsal (bone behind great toe). They include cutting a wedge out of the bone (base wedge), making a semi-circular cut and rotating the bone (crescentic osteotomy) and fusion of joint behind great toe joint (Lapidus bunionectomy). Base procedures are usually indicated for a moderate to severe bunion.
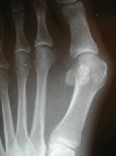
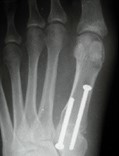
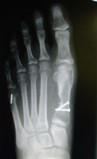
Lapidus and base wedge bunionectomy - procedure performed at the base of the 1st metatarsal.
Overall, there are many variables in selecting a bunion procedure and the key to success is finding an experienced surgeon who understands each variable and delivers exceptional results each time.
There is substantial medical research showing which bunion procedures are most effective in specific situations. At CPSM, we perform an examination of your lower leg and foot, review your biomechanics and x-rays, and give you an understandable and complete explanation of what choices you have, including what type of procedure is in your best interest.
Who Should Perform Your Surgery?
The most important criteria to ensure good outcome for your bunion surgery is to choose the right surgeon. The qualities that make for a good bunion surgeon are:
- Understanding of biomechanics: To choose the best procedure, a surgeon must also can evaluate your biomechanical structure including tightness of leg muscles, foot and leg alignment, motion of the bones around the bunion site, and midfoot and rearfoot alignment. He should be assessing your posture and walking. Some of the critical assessments are done during the procedure. This is probably the most important factor of all
- Extensive experience: An experienced surgeon usually has a better ability to deal with intra-operative or post-operative complications and reduce the chance of complications. A god care of you and a close observation of your post-operative progress is equally critical
- Gentle handling of tissue: A surgeon who handles tissue with a gentle touch will help ensure that pain is minimised and recovery time is reduced. Often a fast surgeon is not necessarily a better one
- Defines realistic expectations and potential problems: Make sure you discuss all possible complications with your surgeon
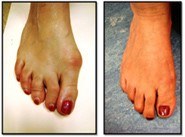
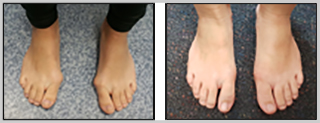
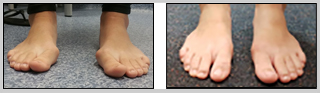
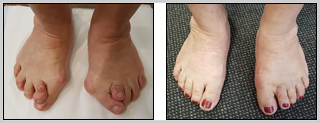
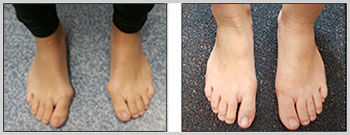
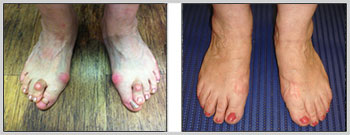
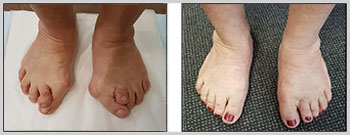
SELECTION OF CASES
- Immediate After Surgery
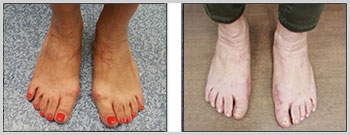
- Bunion Surgery – 4 weeks follow up
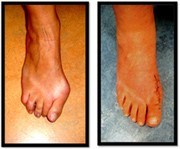
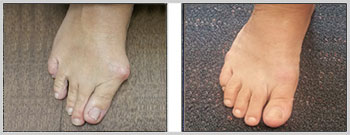
- Bunion Surgery – 8 weeks follow up
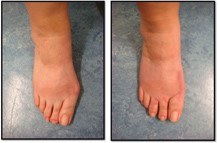
- Bunion Surgery 3 – 8 weeks follow up
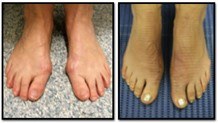
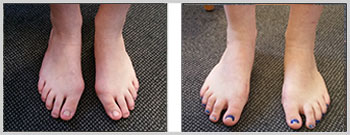
- Bunion Surgery 2 – 5 years' follow-up